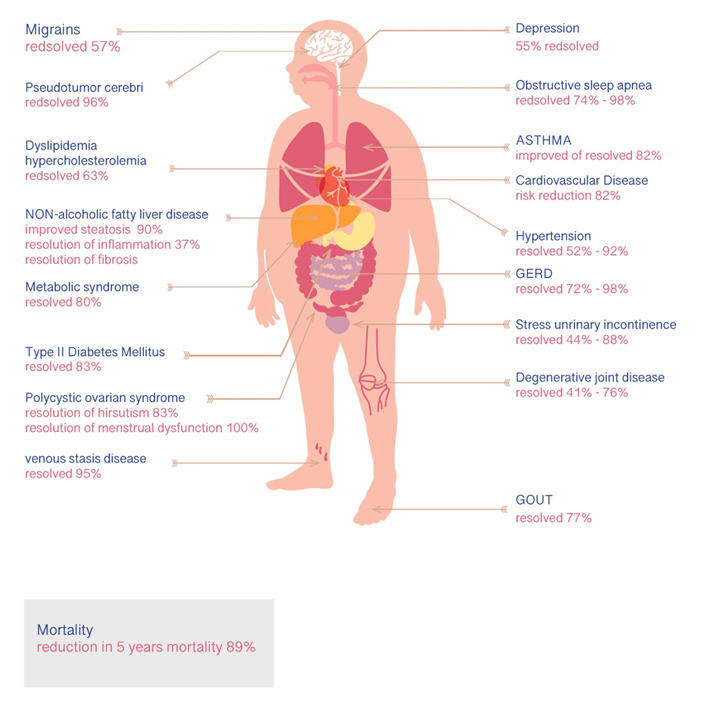
Benefits of Bariatric Surgery:
Quality of Life
- Obesity is associated with impairments in quality of life. In particular, obesity can cause increased physical limitations, bodily pain, and fatigue.
- The National Health and Nutrition Examination Survey found that morbidly obese women (BMI >40 kg/m2) were four times more likely to be depressed as women with a normal BMI.
- Numerous studies have suggested that individuals report improvements in psychosocial functioning with weight reduction. The most consistent finding in this area is the association between surgical weight loss* and improved quality of life.
- More than 95% of the patients who had bariatric surgery at our center reported markedly improved or improved quality of life after surgery in an anonymous survey.
- Obese patients who had bariatric surgery not only live longer, but also live much better.
*Weight loss results can vary depending on the individual. There is no guarantee of specific results
Diabetes Mellitus
- Obesity is a major independent risk factor for developing type 2 diabetes, and more than 90% of type 2 diabetics are overweight or obese.
- It has been estimated that the risk of developing Type 2 diabetes is increased 93-fold in women and 42-fold in men who are severely obese rather than of healthy weight.
- Diabetes is the leading cause of kidney failure, non-traumatic lower-limb amputations, new cases of blindness among adults, and it is associated with increased risk of: heart disease and stroke, high blood pressure, nervous system disease, kidney disease, blindness, amputations, pregnancy complications.
- The mini gastric bypass and sleeve gastrectomy are effective interventions for treating type 2 diabetes. Improvement in metabolic control is often evident within days to weeks following surgery, most likely reflecting an alteration in metabolism that is independent of weight loss.
- Data show that the longer the duration of diabetes, the less chance to have remission after bariatric surgery. That means the sooner to have bariatric surgery, the better chance to have remission of diabetes for obese patients.
- Meta-analysis of 22,000 bariatric surgery patients in 136 studies (1990-2003) found 86% of patients saw improvement or resolution of type 2 diabetes.
- American Diabetes Association recommends bariatric surgery be considered for adults with type 2 diabetes who have a BMI greater than 35, in particular if diabetes or associated co-morbidities are difficult to control with lifestyle and pharmacologic therapy.
Fatty liver disease
- Nonalcoholic fatty liver disease (NAFLD) is one of the most common causes of chronic liver disease worldwide, and morbid obesity is strongly associated with its development. NAFLD is subdivided into nonalcoholic fatty liver (NAFL), hepatic steatosis without inflammation, and nonalcoholic steatohepatitis (NASH), which is associated with inflammation and can be indistinguishable histologically from alcoholic steatohepatitis.
- The general approach to the overweight or obese patient with NAFLD or NASH is lifestyle modification and weight loss.
- Although it was a rare indication for liver transplant 20 years ago, NSAH now is No.2 reason for people to get liver transplant. It is estimated that it will be the No.1 reason for liver transplant in the near future with the epidemics of obesity.
- There is no good treatment for NASH except weight lose. Bariatric surgery has been shown to be the most effective ways to slow down or reverse the progression of NASH. Studies have shown more than 80% of resolution of NASH after bariatric surgery.
Hypertension and Hyperlipidemia
- Bariatric surgery was reported to cause normalization of hypertension in 30-50% of patients with medication and reduced need of antihypertensive treatment in a further 20-30% of patients.
- Patients with complete resolution of hypertension after surgery usually had a shorter duration of hypertension compared with patients without resolution. That means the sooner to have bariatric surgery, the better chance to have remission of hypertension for obese patients.
- Up to 50% of morbidly obese patients who undergo bariatric surgery have dyslipidemia.
- Large studies show that bariatric surgery leads to resolution of dyslipidemia in about 60% of the patients.
- Bariatric surgery leads to close to 50% reduction of heart attack risk and more than 50% reduction of stroke risk.
Joint Pain and Osteoarthritis (OA)
- Most patients with OA develop join pain involving weight bearing joints including lower limb and back pain.
- Studies have demonstrated that among patients with knee OA pain, bariatric procedures can predictably provide relief. Dramatic reductions in pain can occur as quickly as three months post-surgery
- Retrospective studies have revealed that the frequency of back pain was reduced in up to 83% of patients, and lumbar back pain symptoms were reduced in 82–90% patients after 6–22 months.
Obstructive Sleep Apnea
- Weight loss and continuous positive airway pressure (CPAP) therapy are the cornerstones of therapy for sleep apnea.
- A meta-analysis of 69 studies and 13,900 obese patients performed in 2013 identified a high rate of resolution or improvement in OSA following bariatric procedures.
Obesity Associated Cancer
- Large epidemiology studies have shown that obesity confers an increased risk to various malignancies including cancers of the colon, gallbladder, endometrium, breast and pancreas.
- Bariatric surgery has been shown to reduce the risk of developing new cancers.
- A large retrospective study from Canada showed nearly 80% reduction of cancer incidence after bariatric surgery.
Polycystic Ovary Syndrome and Infertility
- Polycystic ovarian syndrome (PCOS) is the most common endocrine disorder in women. It is strongly associated with obesity. It is found in 30 percent to 70 percent of obese women of reproductive age and is associated with irregular period, excessive hair and a high risk of infertility.
- For PCOS patients with infertility, bariatric surgery also has been shown to increase the fertility rate.
- Even in women with regular menstrual period, observational studies have shown obesity is associated with decreased spontaneous pregnancy rates and increased time to pregnancy.